6 Myths About Addiction
Many people don’t understand addiction and substance abuse or dependency. They think those who struggle with addiction must lack moral substance or willpower. In reality, breaking the cycle of addiction takes far more than an iron will or even a desire to quit. Addictive substances and behaviors quite literally alter the chemistry of the brain and make quitting extremely difficult- though not impossible.

Is Addiction a Disease?
Addictions Alter Brain Chemistry Making Quitting Difficult- Not Impossible
I remember a time, before my career as a counselor, when I was volunteering at a church and attended a funeral where the deceased had died of an overdose. He was only 21 years old. I remember thinking, “Well, that’s what happens when you make poor choices.” But then the father of the young man shared with deep heartfelt sorrow that, “Addiction is a disease, a disease my son couldn’t beat.” Hearing that statement caught me off guard.
A disease? How can you compare addiction to a disease? No one chooses the disease of cancer, no one chooses the disease of Alzheimer’s. Addiction isn’t a disease because he could have said no but he chose not to.
Harsh? Yes. Looking back I’m ashamed I couldn’t see past my own judgements about addiction to have compassion for the family. They had just lost their son and I scoffed at how he died.
Looking forward, my first job within the world of mental health was at a residential treatment facility for eating disorders. This is really where my perception of addiction started to shift. Eating disorders are an addiction related to an unhealthy relationship with food where the individual is either obsessively restricting, binging, planning out their next meal, or figuring out a way to get rid of the calories they just ate. (You can read more about that here). This experience taught me that while much of the illness is about the food, it’s also about so much more. I learned that addiction can truly be a disease.
There are many myths about addiction that, if believed, can keep the people we are trying to support stuck and keeps those around them reliving hurt time and time again. Here are a few:
Myth 1: They chose to do it, so if they get addicted it’s their fault
Yes our choices lead to outcomes, sometimes intended, sometimes unintended. By the time a person has gotten to the level of an addiction, it isn’t as simple as choosing or not choosing. When a person crosses from abuse to a true addiction, it develops from of a history of unhealed pain- pain that is fueled over time by shame.
Shame is the painful experience of feeling a mixture of regret and self-hate. It’s the feeling that doesn’t just say what you did was bad, but who you ARE is bad. When shame takes root, it grows and festers like a cancer. As it grows, so does the need for the substance to match its pain as a way to numb it. It’s why some people can be around alcohol and have no issues and some people can’t go a day without it. It’s not always genetics, though that can play a part. The substance provides immediate but temporary relief to deep wounds and gives a rush of dopamine and euphoria. The person may not even be aware those wounds exist. It’s that temporary “high” that keeps people coming back, and slowly the brain becomes dependent on the substance as the primary way to cope with life stressors.
As shown below, there is a progression of dependency that leads to the level of addiction. Many people never reach the level of an addiction, but those who do have certain risk factors that can lead to an addiction. (1)
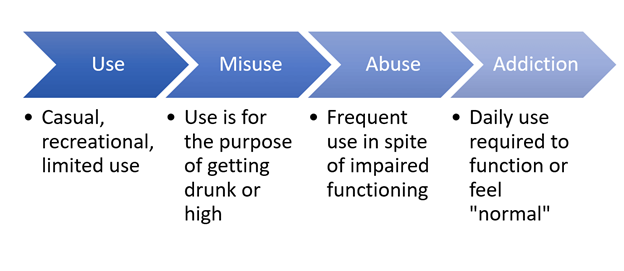
Myth 2: People have to hit rock bottom before they get better
This is both untrue and dangerous. Hitting rock bottom can look like a lot of different things, but in its most horrible form, rock bottom can be deadly. It’s the point a person reaches when they have nothing more to lose. While pain is a strong motivator, it’s not the only type of motivation. Just because a loved one hasn’t hit their “rock bottom” yet doesn’t mean you have to wait until they do to get help.
It’s much less time consuming, expensive, and emotionally damaging to treat an addiction that hasn’t reached the worst place than it is for someone who has gone too far. Not intervening because someone hasn’t hit their rock bottom can enable the abusive behavior.
I’ve also heard people use their lack of consequences as a way of gaging their substance use to rationalize their behavior “isn’t as bad” comparatively speaking. Just because you haven’t experienced consequences from behavior, doesn’t mean consequences aren’t happening. People with addictions often believe their substance use isn’t hurting the people around them. Emotional and psychological consequences are being experienced by the people in the person’s life. These consequences can have damaging and long-lasting impact.
Myth 3: You can’t force someone into treatment or counseling, they have to want it.
It is true a person does have to see the need to change before deciding to actively get help, but regardless of where a person is in their stage of desire to change, they can still receive some benefits of going to treatment or counseling. Depending on how destructive a person’s behaviors are, requesting that they receive counseling or treatment in a loving way can be an appropriate boundary not just for their protection but for the people in their life. I tell people that it doesn’t matter how they get there, it just matters that they’re there. People can change the way they think about their addictions even if they go to counseling believing they don’t have a problem.
I used to work with adjudicated youth that were often mandated to participate in counseling either by their probation officer or by the judge. Either way, when they finally landed in my office, they didn’t want to be there nor did they believe they needed to be there. I didn’t try to change that or convince them otherwise, my main objective was just to provide a safe place to talk. Over time, they would often come to enjoy coming to counseling because it became a safe place to process and share.
People who struggle with addictions have learned to suppress their emotions and numb them out. Counseling can be the first step of learning to sit with emotions and process what they are feeling without resorting to numbing.
Myth 4: Going to treatment will fix the problem
This may seem obvious, but I can’t tell you how many times either people with addictions or their family members get discouraged when a relapse happens after treatment or throughout counseling. They are frustrated that they spent an abundance of money, time, and energy just to feel like it was all “pointless” or “it didn’t work.” But bigger than that, it can feel deeply personal. Like, “they don’t love me enough to stop.”
When I worked for the eating disorder center, it was common for women to graduate treatment, move on to the next phase, then come back and have to “start all over”- sometimes 2-3 times. Cycles happen in addiction and you can expect relapses to happen, but that doesn’t mean they aren’t trying or that it has anything to do with the people they care about. It takes a long time for the brain to become dependent on substances/behaviors, so you can expect a long time for the brain to heal itself.
Treatment and/or counseling is step 1 in a multifaceted approach to bring change. When healing an addiction, changes also need to be made to the addict’s environment. How they structure their day, the people they surround themselves with socially or professionally, family support and dynamics can all play a role in contributing to a relapse or remaining addicted.
Myth 5: If they relapse it means they’re not getting better
With drug addictions specifically, 40-60% of people relapse even in active treatment. (drugabuse.gov) “When a person recovering from an addiction relapses, it indicates that the person needs to speak with their doctor to resume treatment, modify it, or try another treatment.” In other words, with each relapse there can be a new learning experience and “blind spot” to be addressed. Especially as a loved one of someone struggling with an addiction, approaching a relapse as a learning experience. Rather than expressing disappointment and condemnation, try to create safety for the addict to approach you in the future and not add to the level of shame of relapsing again.
Shame is the ultimate enemy in recovery, and it comes in many forms. Shame can look like defensiveness and attacking back, it can look like withdrawal and isolation, it can even look like pride and dismissal of behavior. So, instead of paying attention to the destructive behaviors that happened in the relapse, try to understand what was working up until the relapse and why it failed.
When looking at what happened in a relapse, the person may think they are getting worse or feel stuck, which leads to discourement and hopelessness. Focusing on what was working and what maybe got easier or better allows an addict to stay motivated and hopeful that their hard work is paying off. It’s important not to dismiss what happened in a relapse; taking ownership is vital to everyone involved but dwelling on it does not change behavior long term.
Myth 6: An addict is always an addict
It is true that drugs and alcohol change a person’s brain on such a level that the goal has to be managing symptoms rather than curing the disease. When a person experiences an addiction, their brain conditions itself to depend on their substance of choice. So, like muscle memory, it wouldn’t take long to develop an addiction towards something else- it’s quite common for addictions to shift to another behavior. The brain likes familiarity and its first inclination is to go toward the familiar. This inclination does not mean a person will always be an addict, but it does mean they must always be aware of their behaviors and motivations.
My perception of addiction has changed over the years. I believe that these truths about addiction are important to understand:
- Addiction isn’t personal and is a symptom of something that was years in the making.
- The most important skill in addiction recovery, for both the addict and their support people, is 100% honesty. Protecting one another from feelings or addictive behaviors will only result in relapse and long term resentment.
- Addiction isn’t anyone’s responsibility to fix except for the person who has the addiction. Trying to step in and “help” can easily turn into an unhealthy dependance on you.
- Giving the power to choose is the biggest demonstration of love. Giving an addict permission to choose their addiction doesn’t mean you’re enabling the behavior as long as you are able to set clear boundaries for yourself and the relationship.
- Knowledge is power with addiction. Understanding the physiology of how addiction changes the brain helps combat the shame of not being good enough to stop it.
- Shame is the ultimate enemy. Shame makes it impossible to believe you are worth recovery and keeps you in the cycle of addiction.
- A marriage doesn’t have to end if a spouse has an addiction. Marriages end when both people aren’t willing to work on themselves to change the dynamics of their relationship.
There is help and recovery from addiction is possible- no matter what the substance or behavior is. Counseling is a great first step to help give you the tools to combat addiction.
This article was written by Emilie LeLaCheur. Emilie is no longer with New Life Counseling.
Citations
- Resources. (n.d.). Retrieved March 26, 2021, from https://signalbhn.org/resources/
- NIDA. 2020, June 3. How effective is drug addiction treatment?. Retrieved from https://www.drugabuse.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition/frequently-asked-questions/how-effective-drug-addiction-treatment on 2021, March 26
- NIDA. 2020, July 10. Treatment and Recovery. Retrieved from https://www.drugabuse.gov/publications/drugs-brains-behavior-science-addiction/treatment-recovery on 2021, March 26

